Laser Eye Surgery and Glaucoma: Understanding the Safety of MyLumineyes®
A common concern for those considering permanent eye color change is the potential risk of Glaucoma. Since the procedure involves iris pigments, understanding how these pigments interact with your eye’s natural drainage system is vital for long-term safety. On this page, we can look for the answer to the question of whether Lumineyes, unlike other methods, actually causes glaucoma.
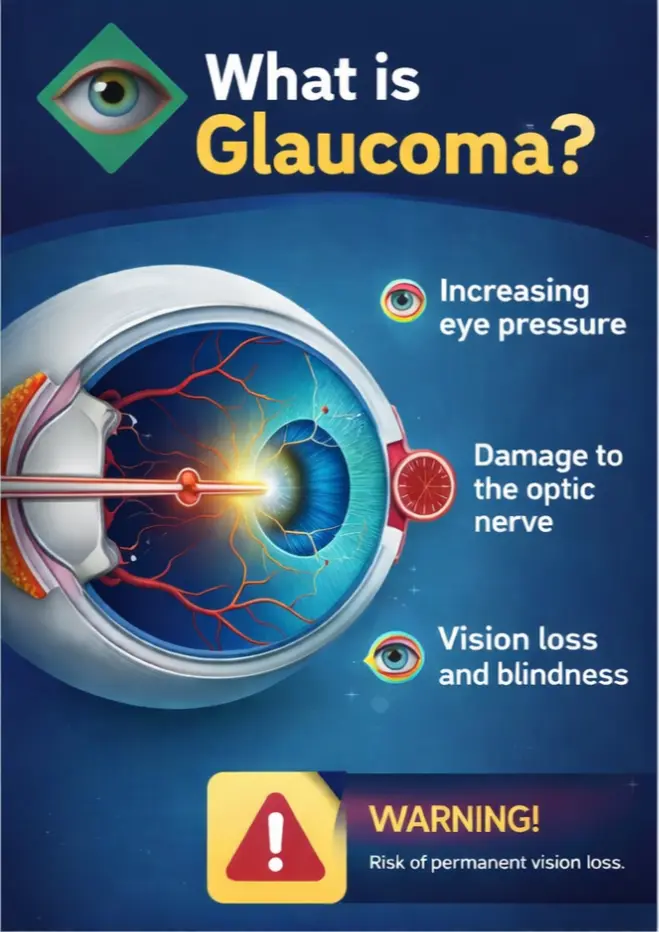
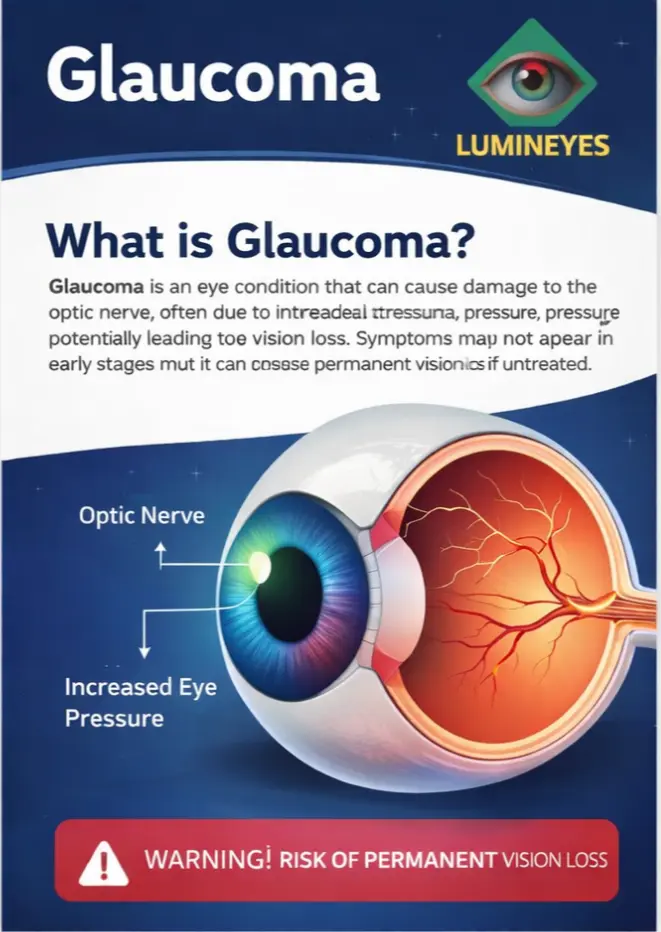
What is Glaucoma in the Context of Laser Treatment?
Glaucoma is typically caused by increased intraocular pressure (IOP), which happens when the eye’s drainage angle (trabecular meshwork) becomes blocked. In lower-quality laser procedures, pigments are released too quickly, potentially clogging these pathways[cite: 3]. This is why staged treatment and professional monitoring are non-negotiable for safety.
How MyLumineyes® Protects Your Eyes Against Glaucoma
As the inventor of this technology, Dr. Mustafa Mete developed the MyLumineyes® protocol specifically to eliminate these risks. Our approach focuses on selective photodisruption, meaning we target only the superficial melanin without harming deeper tissues[cite: 3].
Comparison: Why Safety Depends on the Protocol
| Feature | Commercial Clinics | MyLumineyes® Protocol |
|---|---|---|
| Laser Energy | High (Aggressive) | Low-Intensity & Selective |
| Pigment Clearance | Sudden & Unmonitored | Staged & Gradually Managed |
| IOP Monitoring | Often Ignored | Continuous Clinical Tracking |
As shown in the table above, Lumineyes works on a different principle than other methods, and our studies have shown that it does not cause glaucoma. For our article on the safety of laser treatment, see: [safety of laser eye color change]
Can Someone with Existing Glaucoma Have the Procedure?
Integrity and medical ethics come first at MyLumineyes®. Individuals with active or advanced Glaucoma are generally NOT suitable candidates for laser eye color change[cite: 6]. A thorough examination of your drainage pathways and iris structure is required to determine eligibility[cite: 3].
⚠️ The Danger of “Rapid” Sessions
Promising immediate results or fixed “short-term” packages is dangerous. Forcing rapid pigment change can overload the eye’s natural drainage, leading to irreversible Glaucoma. We strictly pace our treatments according to your individual biological response to ensure your vision remains protected[cite: 13, 14].
Key Safety Takeaways
- Individualized Session Planning: Treatment duration is adjusted based on your pigment grade[cite: 5, 13].
- Noticeable Changes: Initial results typically appear within 4-6 months, allowing the eye to adapt safely[cite: 14].
- Expert Supervision: Every step is managed by Dr. Mustafa Mete, ensuring 15 years of safety data is applied to your case[cite: 1, 13].
For more detailed information on pricing and risks, please visit our Cost and Risks page or read our Disclaimer.