Eye Color Change Method Comparison 2026
People often use the phrase eye color change to describe very different approaches. However, these methods are not medically equivalent. Some are temporary and cosmetic, while others involve structural or pigment-related intervention. The most meaningful differences are not only visual outcome, but also reversibility, follow-up requirements, and long-term ocular considerations.
This page provides a structured comparison of the main eye color change methods without treating them as interchangeable options. Instead of focusing on marketing claims, it looks at how each method works, whether the effect is temporary or long-lasting, what type of monitoring may be required, and where the main limitations usually appear.
Why a Comparison Page Matters
Many online discussions place all eye color change options into the same category. In reality, cosmetic lenses, iris implants, and pigment-reduction approaches differ greatly in both mechanism and clinical implications. A person exploring these options should not assume that every method carries the same level of intervention, reversibility, or follow-up burden.
A useful comparison should therefore go beyond appearance alone. It should clarify how the color change is produced, whether the effect depends on a foreign material, whether the eye’s anatomy is structurally altered, and whether continued medical supervision is required.
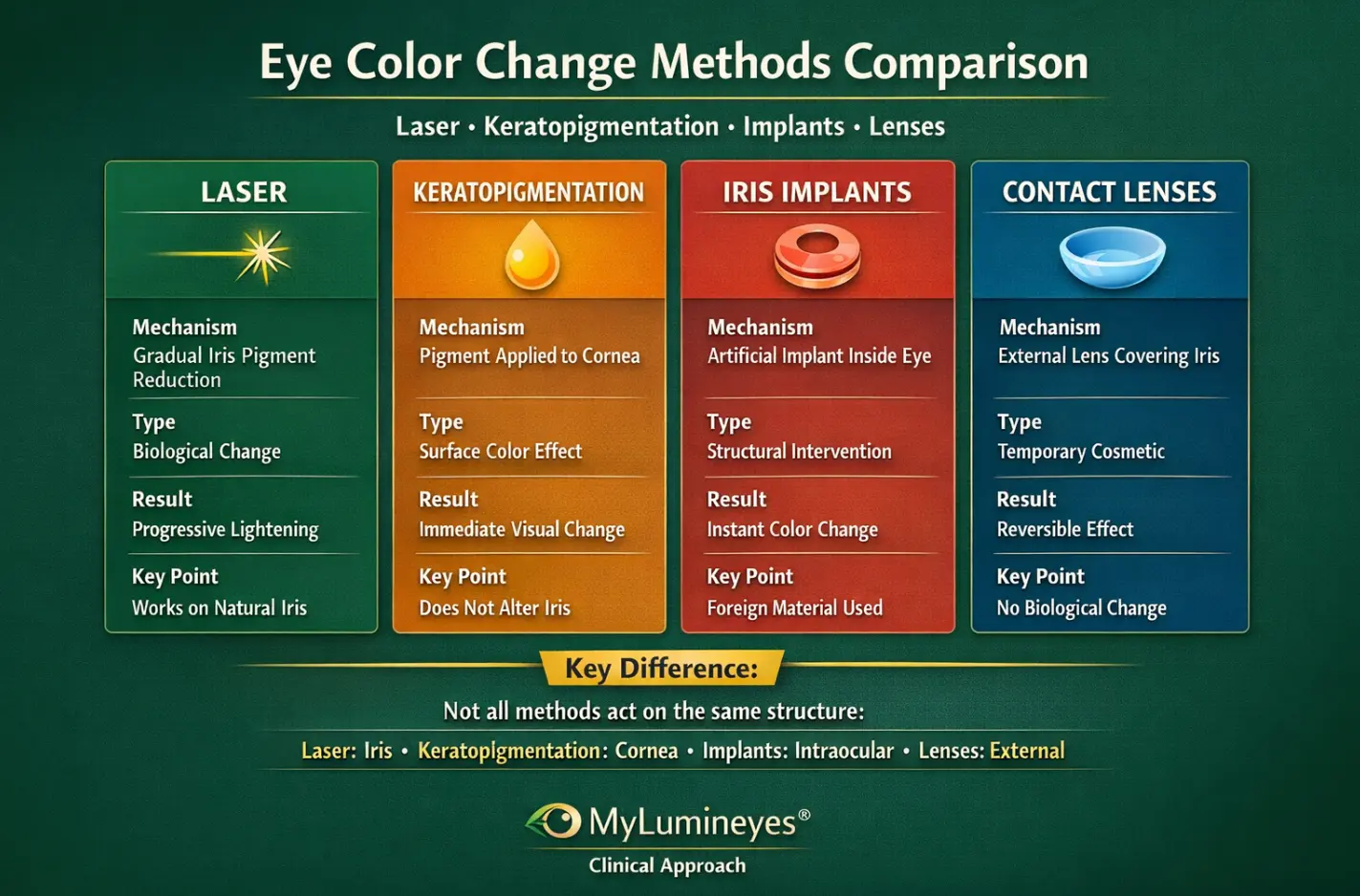
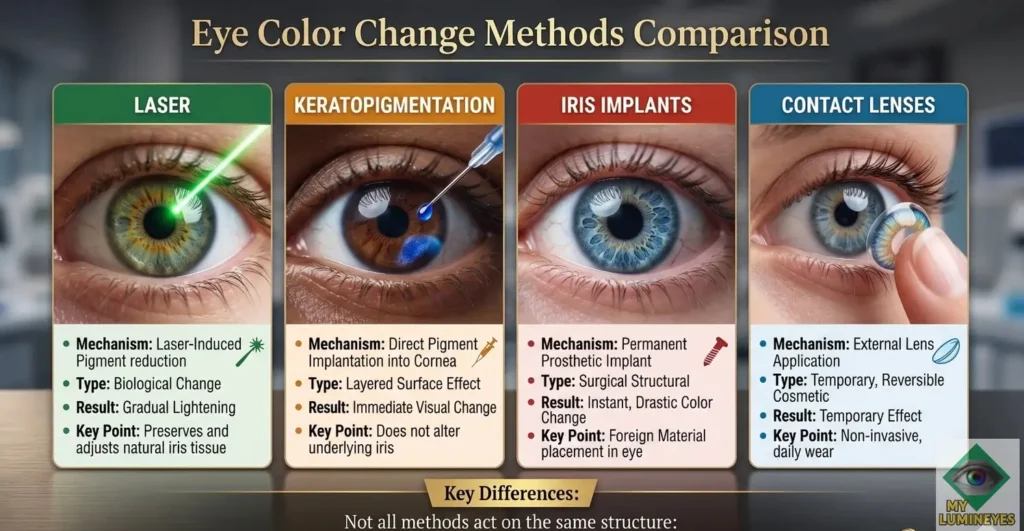
* This infographic illustrates how different eye color change methods vary in mechanism and anatomical target. While laser approaches act on iris pigment, keratopigmentation affects the cornea, implants involve intraocular structures, and contact lenses provide a temporary external effect.
Main Eye Color Change Methods
1. Laser Pigment Reduction
Laser pigment reduction or depigmentation is based on the gradual reduction of superficial iris pigment. Rather than inserting an artificial material or placing a cosmetic device inside the eye, this method aims to reduce visible pigment density over time through staged treatment planning. The visible transition is typically progressive rather than immediate, and the final outcome depends on baseline pigment density, iris biology, and treatment response.
2. Artificial Iris Implants
Artificial iris implants are intraocular devices placed inside the eye. Although they can create an immediate visual color change, they are fundamentally different from pigment-reduction approaches because they rely on a foreign implant rather than biological lightening. Their mechanism, reversibility profile, and structural implications should not be evaluated as if they belong to the same category as non-implant methods.
3. Cosmetic Contact Lenses
Cosmetic contact lenses create a temporary visual color change by covering the natural iris appearance. They do not biologically alter iris pigment and do not permanently change eye color. Their role is cosmetic and reversible, but safe use still depends on proper fitting, hygiene, and appropriate lens practices.
4. Digital or Temporary Cosmetic Simulation
Digital filters, photo editing tools, and eye color simulators can preview possible visual outcomes, but they do not represent a medical result. These tools may be useful for visualization and consultation planning, yet they should never be confused with a clinical treatment or a predictor of a guaranteed final shade.
5. Corneal Keratopigmentation
Corneal keratopigmentation is a technique in which pigment is applied within the corneal layers to alter the apparent color of the eye. Unlike pigment-reduction approaches, this method does not change the natural iris itself, but instead creates a visual effect through corneal coloration.
Because the mechanism involves the cornea rather than the iris, the result is based on surface-level optical modification rather than biological pigment reduction. This distinction is important when comparing it to other approaches, as the underlying anatomical structures involved are different.
Eye color change method comparison and options
| Method | How It Works | Temporary or Long-Lasting | Medical Supervision | Main Limitation | Follow-Up Need |
|---|---|---|---|---|---|
| Laser Pigment Reduction-Laser eye color change | Gradual reduction of superficial iris pigment through staged treatment | Intended to be long-lasting in appropriate candidates | Yes | Outcome depends on biology, pigment density, and treatment planning | Structured monitoring required |
| Artificial Iris Implants | Placement of an intraocular artificial device to create color change | Long-lasting unless removed | Yes | Relies on a foreign implant and should not be considered equivalent to pigment reduction | Ongoing clinical evaluation may be necessary |
| Cosmetic Contact Lenses | Masks the natural iris color with an external lens | Temporary | Not always medically supervised, but proper fitting is important | No biological color change occurs | Depends on usage pattern and lens hygiene |
| Digital Simulation | Creates a visual preview using software or image processing | Temporary | No | Does not represent a medical outcome | No clinical follow-up |
| Corneal Keratopigmentation | Pigment applied within corneal layers to create a color effect | Long-lasting visual effect | Yes | Does not change iris pigment, effect is corneal-based | Clinical follow-up required |
Why These Methods Should Not Be Treated as the Same
One of the most common mistakes in online discussions is to compare all eye color change methods as if they belong to a single category. In reality, they differ at the level of mechanism, reversibility, structural involvement, and biological response.
For example, a method based on pigment reduction does not function in the same way as a method based on inserting an implant. Likewise, a temporary cosmetic lens should not be evaluated using the same framework as a medically supervised clinical intervention. Even if the visual goal appears similar, the path to that result is fundamentally different.
This distinction matters because the eye is not a cosmetic surface alone. It is a delicate biological system, and the route by which color change is attempted has direct relevance to changing eye color safety considerations, follow-up design, and long-term stability, particularly in terms of potential risks such as irritation, infection, or damage to the eye structure. It is absolutely essential that you are fully aware of the risks involved in eye color change procedures.
What Should Be Compared First: Appearance or Mechanism?
From a clinical perspective, mechanism should always be evaluated before appearance. A visually attractive result does not by itself explain how that result was created, whether it depends on a removable device, whether tissue response is involved, or whether follow-up remains necessary after the initial treatment period.
For this reason, a meaningful comparison should begin with questions such as:
- Does the method rely on a foreign material?
- Is the color change biological, optical, or device-based?
- Is the result temporary, removable, or intended to be stable over time?
- What type of monitoring is needed before and after the intervention?
- Does the method require a structured medical framework?
Temporary vs Long-Lasting Approaches
Temporary options, such as cosmetic contact lenses or digital simulations, may be suitable for people who want visual experimentation without a biological change. Their effect disappears when the lens is removed or the simulation is closed.
Long-lasting approaches are different because they are not based on temporary external masking. They require a more serious evaluation of patient suitability, long-term expectations, and clinical follow-up. This is why the discussion should not focus on color alone, but on whether the chosen method aligns with the person’s medical profile and expectations.
The Role of Medical Supervision
Medical supervision is one of the clearest dividing lines between simple cosmetic options and true clinical interventions. A medically supervised method involves preoperative evaluation, treatment planning, interval control, and post-treatment monitoring. This is particularly relevant when pigment behavior, intraocular pressure, or anterior segment balance may influence treatment decisions.
By contrast, non-medical cosmetic options may create a visible effect without changing ocular biology. That distinction should remain clear throughout any serious comparison.
Why Oversimplified Comparisons Can Mislead Patients
A simplified online chart may suggest that all eye color change methods differ only by convenience or price. That is rarely a clinically useful way to compare them. The real questions involve biological mechanism, reversibility, structural involvement, and monitoring demands.
Patients should therefore be cautious with comparisons that focus only on appearance, promises, or broad marketing language. A responsible comparison should help separate cosmetic masking from biological pigment change, and non-invasive visualization from intraocular intervention.
Clinical Interpretation
The key takeaway is that eye color change methods are not interchangeable. A temporary lens, an implant-based approach, and a staged pigment-reduction pathway should not be discussed as if they carry the same implications for the eye.
For patients seeking a medically structured understanding, the most important comparison points are not dramatic claims or before-and-after impressions alone. They are mechanism, permanence profile, follow-up design, and the extent to which the method respects ocular physiology over time.
Related Clinical Guides
If you would like to explore the laser-based approach in more detail, the following pages provide a more focused explanation:
- How the laser-based eye color change process works
- The Dangerous Illusion of Authority in Laser Eye Color Change
- Cost and risk overview
- Before and after examples
- For broader biomedical literature, see PubMed.
Conclusion
Comparing eye color change methods requires more than looking at visual outcome alone. The most important differences lie in how the change is created, whether the effect is temporary or intended to be stable, and what kind of medical framework surrounds the process. When these factors are understood clearly, patients can make more informed decisions and avoid treating fundamentally different methods as if they were the same.