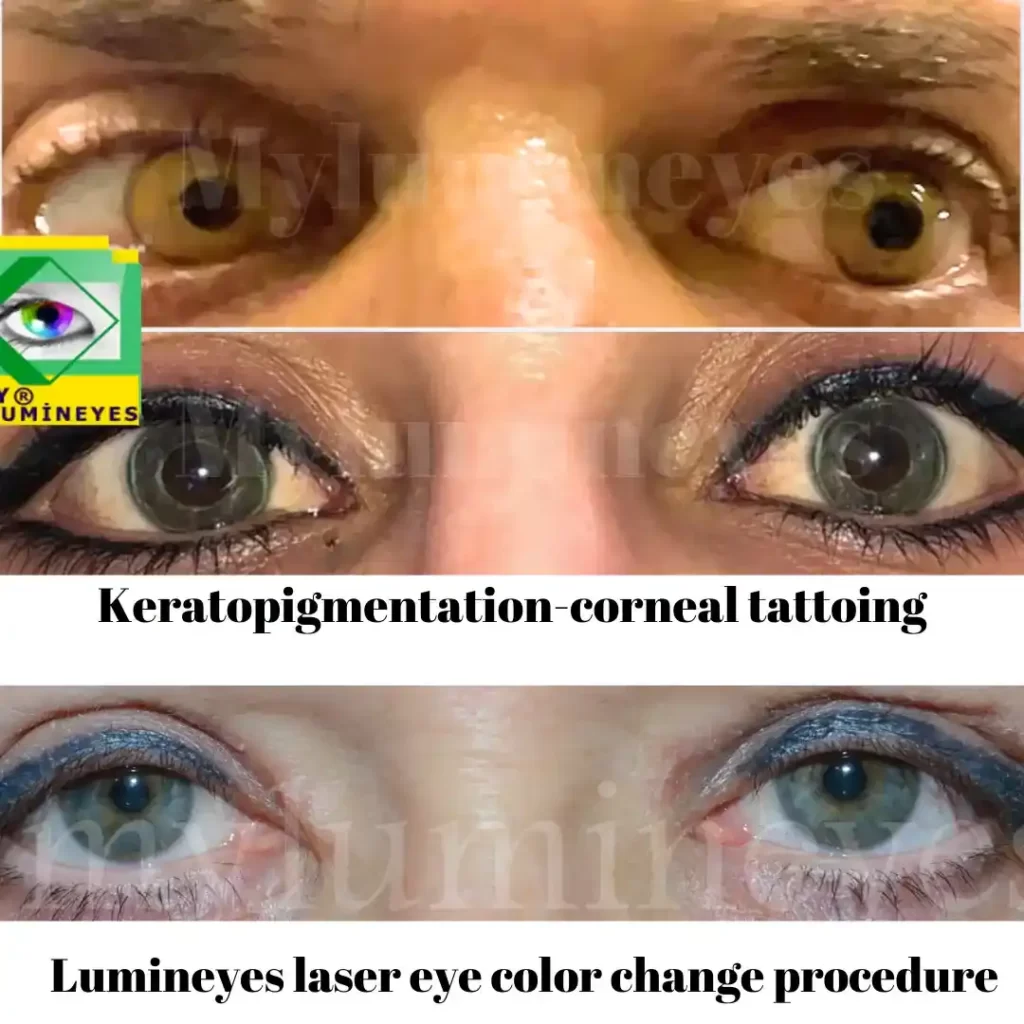
Keratopigmentation Risks and Long-Term Complications
Keratopigmentation is a corneal tattooing technique in which pigment is inserted into the corneal stroma to simulate a new iris color. Although it can create an immediate cosmetic effect, the procedure alters the cornea—one of the eye’s most important optical structures. Because of this, keratopigmentation may lead to significant short-term and long-term complications, some of which may not be fully reversible.
For patients looking for non-incisional, medical alternatives, you may review our main page:
Laser Eye Color Change.
To understand how keratopigmentation differs from the cosmetic version of the procedure, you may also see:
Keratopigmentation Eye Color Change.
What Happens Inside the Cornea During Keratopigmentation?
The procedure involves depositing synthetic pigment into channels or tunnels created within the corneal tissue. Because the cornea is responsible for optical clarity, refractive function, and regular curvature, any pigment placement may disrupt these properties. The effect may look uniform immediately after the procedure, but pigment stability and tissue response vary widely between individuals.
1. Early (Short-Term) Complications
Pain, Light Sensitivity and Surface Irritation
Corneal nerve irritation following channel creation or pigment placement can cause acute discomfort, tearing, photophobia, and burning sensations.
Inflammation or Iritis
Pigment particles may trigger inflammatory responses inside the eye. Even minor inflammation can affect vision quality or induce temporary intraocular pressure fluctuations.
Irregular Healing of the Corneal Tunnel
If tunnel healing is incomplete or uneven, corneal shape may become irregular, contributing to blurred or fluctuating vision.
Foreign Body Sensation
Some patients experience persistent dryness or a sensation of roughness due to corneal surface disruption.
2. Long-Term Structural and Optical Changes
Permanent Reduction in Visual Quality
Patients may report decreased clarity, glare, starbursts, or haloes—especially at night. These issues can persist even if part of the pigment fades with time.
Irregular Astigmatism
Changes in corneal thickness, tunnel symmetry, or pigment placement can alter corneal curvature, creating unpredictable refractive errors.
Pigment Stability Problems
Pigment may migrate, break down, or fade irregularly. Areas of uneven coloration can produce patchy cosmetic appearance that is difficult to correct.
Challenges in Future Ophthalmic Care
Cataract surgery, glaucoma assessment, or retinal evaluation may become more difficult due to reduced optical clarity or altered corneal biomechanics.
3. Glaucoma and Intraocular Pressure Concerns
Keratopigmentation does not directly treat glaucoma, but it may complicate glaucoma management. Corneal thickness changes, pigment-induced haze, or altered corneal biomechanics can make intraocular pressure measurements less reliable.
- Tonometry readings may be inaccurate due to altered corneal rigidity.
- Optic nerve evaluation may be limited if visualization is reduced.
- Angle imaging (e.g., gonioscopy) may become more difficult after pigment placement.
For these reasons, patients with glaucoma or glaucoma suspicion require particularly careful follow-up.
4. Trauma, Emergency Surgery and Foreign Body Management
Any eye can suffer trauma, but keratopigmented corneas carry unique challenges for emergency care:
- Unclear wound borders: Pigment can obscure the limits of corneal lacerations.
- Difficult suture placement: Tissue integrity in pigment-treated areas may be weaker.
- Foreign body detection: Reduced corneal clarity can hinder visualization.
These factors increase the complexity of trauma repair and may worsen prognosis in emergency situations.
5. Chronic Surface Problems: Keratitis and Corneal Degeneration
Some patients develop chronic inflammation, recurrent erosions, or progressive haze months to years after keratopigmentation. These issues may persist even if pigment partially fades.
- Persistent irritation or pain
- Light sensitivity and dryness
- Fluctuating or reduced vision
- Episodes of recurrent keratitis
6. Can Keratopigmentation Be Reversed?
Although partial pigment removal is possible, keratopigmentation is generally considered high-risk and difficult to reverse. Removal often requires:
- Multiple corneal surgeries
- Risk of further thinning or scarring
- Potential need for corneal transplantation
Even after surgical removal, the cornea may not return to pre-procedure clarity due to permanent structural changes. Therefore, keratopigmentation should be regarded as permanent and non-reversible rather than a reversible cosmetic procedure.
7. When to Seek an Expert Evaluation
Patients experiencing pain, new visual symptoms, increased light sensitivity, or changes in color uniformity after keratopigmentation should undergo a complete ophthalmic evaluation. Early assessment is essential to prevent long-term damage and manage complications.
For independent information on eye health and corneal surgeries, consult:
American Academy of Ophthalmology.
Conclusion
Keratopigmentation may produce rapid cosmetic effects, but it carries significant and sometimes irreversible risks. Patients considering eye color change should fully understand these complications and explore non-incisional, medically controlled alternatives before making any decision.
Frequently Asked Questions About Keratopigmentation Risks
Is keratopigmentation a safe and reversible way to change eye color?
Keratopigmentation is a permanent corneal tattoo, not a simple cosmetic filter. Pigment is injected into the corneal stroma and can migrate, fade unevenly or trigger tissue reactions over time. Removing it usually requires additional surgery and may never fully restore the original corneal clarity, so it should not be considered a harmless or easily reversible procedure.
What happens if I need cataract or retina surgery after keratopigmentation?
Any future intraocular surgery becomes more complex after keratopigmentation. Biometry and intraocular lens calculations may be less reliable, incisions may have to pass through pigmented areas, and visualization of intraocular structures can be reduced. In some cases, additional corneal procedures or even transplantation may be needed to manage complications.
Does keratopigmentation make emergency trauma surgery more difficult?
Yes. In eye trauma, surgeons need a clear view of the wound edges and corneal structure. Pigment can mask lacerations, make suture placement harder and complicate foreign body removal. This can increase the risk of infection, irregular healing and, in severe cases, permanent vision loss or loss of the eye.
How does keratopigmentation affect glaucoma follow-up?
Keratopigmentation does not treat glaucoma and may complicate its follow-up. Changes in corneal thickness and biomechanics can influence intraocular pressure readings, and pigment-related artifacts can affect imaging of the anterior segment. For a patient who already needs precise, lifelong monitoring, adding an unnecessary corneal tattoo increases uncertainty.
What is the difference between keratopigmentation and MyLumineyes® laser eye color change?
Keratopigmentation tattoos the cornea with pigment to mask the iris, altering a transparent and functional tissue. MyLumineyes® laser eye color change, by contrast, works on the iris pigment inside the eye without cutting or tattooing the cornea. Our approach is designed to respect ocular anatomy and to minimise additional risk for future surgeries and long-term eye health.